Cataract surgery technology has experienced incredible advancements in the last several years. With the introduction of these new materials and advanced technology, cataract surgery has been pushed past a purely medical procedure to become a refractive or vision-correcting procedure.
At Seibel Vision Surgery, Dr. Seibel is proud to offer safe and effective cataract surgery using advanced technology to restore your vision!
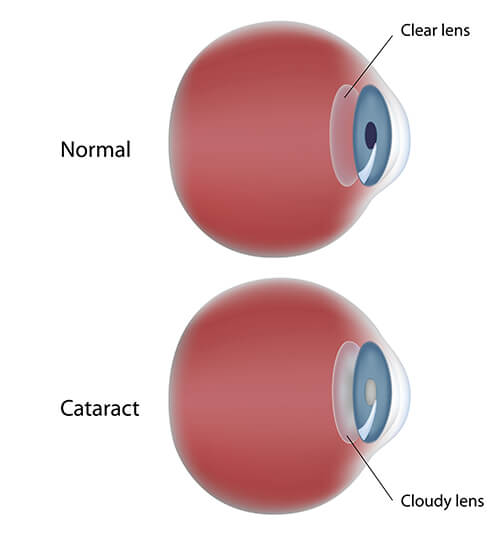
A cataract is a clouding the eye’s natural lens, causing blurry vision, among many other symptoms. More than half of all Americans aged sixty-five and older have a cataract.
Cataracts are a normal part of aging and usually develop over time. Since they typically grow gradually, cataracts often don’t have to be removed when first diagnosed
In the early stages, you may be able to make minor changes to your lifestyle, like stronger lighting or a change in your glasses prescription to combat your cataract symptoms and changing vision. However, at a certain point, cataract surgery may be needed to improve your vision.
Today, cataract surgery is safe and very effective. It is also one of the most commonly performed procedures.
Before recent advancements, cataract surgery was a lengthy procedure and required an extended and confining recovery period. Now, the surgery is a simple outpatient procedure.
The stay at an ambulatory surgery center is just a few hours, and recovery time after surgery is dramatically reduced. Many people enjoy improved vision with greater independence from visual aids within days to weeks after the procedure.
Cataract surgery today is the result of extraordinary technological and surgical advancements that allows millions of people to enjoy crisp and clear vision once again. A true marvel of modern medicine, cataract surgery may restore vision to levels of clarity you may have never thought possible.
Not everyone will experience the same symptoms of cataracts. However, there are some symptoms that are especially common in those who have cataracts.
Common cataract symptoms include poor night vision, a bothersome glare produced by bright lights, painless blurring of vision, and a fading or yellowing of colors. If this develops slowly over a period of years, it might not be immediately noticeable.

However, your vision will eventually become blurry, like looking through a smudgy piece of glass. You might notice that you are becoming more nearsighted and have difficulty reading.
It’s also common that colors do not appear as brilliant as they once did. If you are experiencing cataract symptoms and are looking for a cataract surgeon in Los Angeles, schedule an appointment at Seibel Vision Surgery.
If you need cataract surgery in Greater Los Angeles or Santa Monica, look no further. At Seibel Vision Surgery, we proudly serve these areas with premier cataract services.
Cataract surgery is the only way to remove a cataract and restore vision. There are no medications, vitamins, eye drops, exercises, or glasses that will cause cataracts to disappear.
During cataract surgery, your cataract surgeon will remove the clouded natural lens inside your eye and replace it with a clear vision-correcting intraocular lens implant. This clear intraocular lens, or IOL, is an artificial lens that will correct your natural refractive error and eradicate cataract symptoms.
There are many types of IOLs to choose from. Your cataract surgeon will help you decide which is best for you based on your vision goals, and lifestyle.
The restoration of precious eyesight is accomplished every day at Seibel Vision Surgery. After bringing you into the surgery room, your eye doctor will numb the surface of your eye with eye drops.
First, your cataract surgeon will make a tiny incision in your cornea, the clear front covering of your eye, that typically does not require any stitches. This incision is self-sealing, meaning the eye’s natural internal pressure holds the incision tightly closed allowing the eye to heal without stitches.

Your cataract surgeon will gently break apart your natural lens using ultrasonic vibrations and vacuum out the pieces. Seibel Vision Surgery offers the most modern, state-of-the-art cataract surgical skills, technology, and innovations to achieve your best possible vision. Laser surgery is an option for patients undergoing cataract surgery; Dr. Seibel was a pioneer in bringing this technology to market. The cataract procedure will be customized for each eye of each patient based on the principles in Dr Seibel’s critically acclaimed cataract surgery textbook Phacodynamics.
Next, your cataract surgeon will insert the IOL of your choice and position it to sit correctly in your eye. Once your new IOL is positioned, the surgery will be complete.
The time to consider cataract surgery depends on your individual situation. Although you may not need cataract surgery right away after you are diagnosed, your eye doctor will likely recommend cataract surgery once your cataracts begin interfering with your everyday activities.
Eventually, safety considerations may be a factor as well, as a developing cataract will limit your ability to have a normal, independent lifestyle. Cataracts can be hazardous when they substantially interfere with your ability to see street signs and traffic lights, drive at night, step off curbs or steps, recognize faces, cook, iron, or read medicine labels.
For this reason, it is important to regularly visit your eye doctor at Seibel Vision Surgery in Los Angeles, California. By visiting your eye doctor routinely, they will be able to monitor the development of your cataracts and recommend cataract surgery when needed.
In the eye, light is focused through your using incredibly small muscles. The retina at the back of the eye can consist of a thin layer of photosensitive cells.
In order for you to experience clear vision, the light must land directly on your retina. The retina gathers information from light and sends electrical impulses to your brain.

The brain then translates that into a mental image, allowing you to see. When you have cataracts, some of the light is blocked from reaching the retina.
Similarly, if you have a refractive error like nearsightedness, farsightedness, or astigmatism, the shape of your eye prevents the light from landing directly on the retina. As a cataract becomes denser, it also takes on a brownish hue, resulting in an image that is both blurred and discolored.
Ideally, the lens is transparent and absolutely clear. Once an IOL is in place, it will appropriately refract the light so that it lands on the retina.
Since the IOL is clear, you will no longer experience typical cataract symptoms like glare and halos. Different types of IOLs can provide you with greater visual freedom after the procedure.
Your cataract surgeon will discuss the best lens options for you during your cataract evaluation.
Do you want to learn more about cataract surgery or determine if you have cataracts? Schedule a cataract evaluation at Seibel Vision Surgery in West Los Angeles, CA, today!
At Seibel Vision Surgery, your eyes and vision are of paramount importance. To help you make the most informed decisions regarding the welfare of your vision, we are delighted to be of service and are happy to answer any questions you may have.
Please take the time to familiarize yourself with the information contained on this site. We have compiled it especially for you!
Monday, Tuesday, Wednesday, and Thursday
8:30 a.m. to 3:30 p.m.
Friday
8:30 a.m. to 3:00 p.m.
OUR ADDRESS
11620 Wilshire Boulevard, Suite 711
Los Angeles, California 90025
PHONE
(310) 444-1134
FAX
(310) 444-1130
Learn about cataracts and their treatment
Learn more about CataractsGlaucoma, Macular Degeneration,
Medical Eye Exams, and other